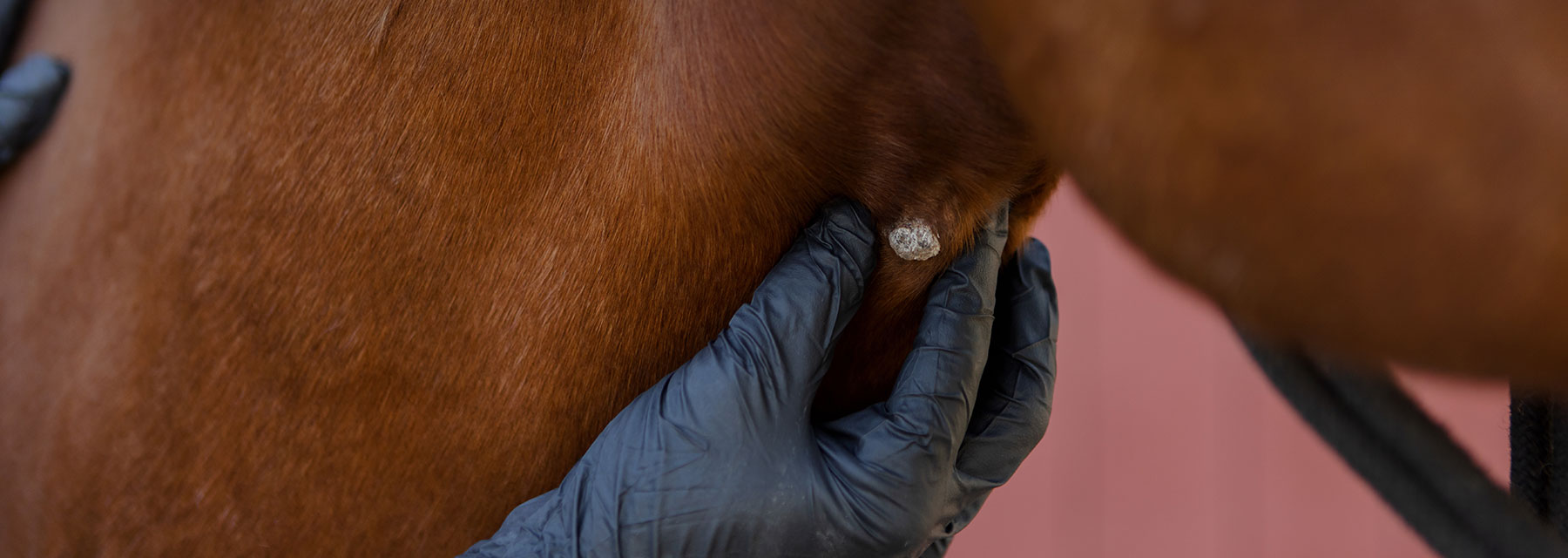
Understanding the Potential Cause, Transmission and Treatment Considerations for a Common and Often Hard to Manage Equine Skin Condition
Sarcoids are a health condition unique to equids — horses, donkeys and even zebras. It is the most common tumor diagnosed in horses, accounting for approximately 90% of equine skin tumors, 40% of all equine cancers and affecting 2% of horses worldwide. These tumors can affect all breeds, ages and sexes. Although sarcoids, also called fibrosarcoma, are locally invasive and recurrent, they do not spread to other organs. They frequently can increase in size, multiply and spread becoming potentially destructive to the animal.
These persistent and progressive lesions can develop anywhere on the skin, but some cutaneous sites are more prone including: the head (especially around the ears, eyes and mouth); chest; underneath the abdomen, sheath and groin; and inside the hind legs. Single or multiple tumors can occur in a specific area or over multiple parts of the body. Sarcoids have an affinity for developing in wounds where they can be confused with exuberant granulation tissue (proud flesh), and are also frequently seen at sites of previous injury and scarring, particularly on the legs. These skin tumors vary considerably in appearance and behavior. Many are non-painful, non-itchy and, especially in early stages, may appear innocuous as smooth, flat or nodular lumps. Some may be completely concealed under the horse’s hair coat. Others, with a dry, scaly, flaky or roughened appearance, look like benign warts. They may have an irregular shape or even a cauliflower-like appearance. The rate at which these tumors grow and, potentially spread, also varies. They range in size from small, slow-growing lesions to large, fibrous masses that grow rapidly to 8-10 cm (3-4 inches) wide. Individually affected horses can develop multiple tumors concurrently and may have a mixture of different types of sarcoids throughout the body.
There is strong evidence that sarcoids are caused by viruses and, although research is continuing, there is currently not a vaccine for equine sarcoids. Another complication is that they do not self-cure and veterinarians do not have a one-size-fits-all method of treatment. If aggravated or subjected to trauma, such as a surgical biopsy, incomplete or failed treatment attempts, or even accidental tack abrasions, sarcoids can become “angry” or more aggressive. Once disturbed, benign tumors may transform into actively growing, ulcerated and damaging lesions. Sarcoids are infamous for high rates of recurrence even after targeted treatments. All of these variables can make it very difficult for veterinarians to successfully treat.
Equine sarcoids are rarely life threatening, but they are costly to owners and a major health nuisance. The financial implications may include high treatment (and retreatment) costs, as well as a reduced resale value of the affected animal. Sarcoids can be very irritating to the horse. As they develop and increase in size, the skin can ulcerate and become open to infection. Particularly in hot weather, ulcerated lesions bleed and attract flies, making it difficult for open sores to heal. If the lesions grow in a location that interferes with tack such as on the face or around the girth area, rubbing can open the lesion causing bleeding and discomfort. This can limit the use of the animal. Although rarely malignant, discomfort from the open wounds, insect irritation or from treatment methods along with frequent recurrence, can significantly affect the horse’s quality of life.
Sarcoids are a health condition unique to equids — horses, donkeys and even zebras. It is the most common tumor diagnosed in horses, accounting for approximately 90% of equine skin tumors, 40% of all equine cancers and affecting 2% of horses worldwide.

Surgical treatments for sarcoids include physical removal, laser surgery and cryosurgery (freezing). Immune modulation treatments may include BCG (bacillus Calmette-Guérin) injections or autologous implantations. Medical management options include chemotherapy, electrochemotherapy, radiation and topical treatments. More than one type of treatment may be used at the same time in combination depending on the sarcoids present.
PHOTOS BY ELIZABETH HAY PHOTOGRAPHY
Causes and Transmission
Strong evidence supports the theory that equine sarcoids are initiated by a viral infection caused by the bovine papilloma virus (BPV), primarily types 1 and 2. There may be a genetic basis for susceptibility in specific horse breeds as current research has identified genetic polymorphisms on several chromosomes associated with sarcoid occurrence. Simply, some breeds or bloodlines may be more likely to develop sarcoids than others. This has been documented in Warmbloods as breeding two sarcoid-affected horses significantly increases the risk for the offspring. Other preliminary breed-related susceptibility has shown Thoroughbreds to be more likely to develop sarcoids than Standardbreds. Lipizzaners, on the other hand, seem more resistant to these skin tumors. It is possible that due to this susceptibility link, sarcoid recurrence is high even in horses that have been successfully treated due to the virus potentially becoming incorporated into the DNA of infected skin cells prompting the transformation into cancer cells. Papilloma viruses in other species, notably in humans, support this.
Current research does not show a significant age, sex or coat color predisposition, although anecdotally it has been suggested that young to middle-aged horses — between 3- to 6-year-olds — are most commonly affected with a majority of cases, and that gelded horses appear more frequently affected.
While the mode of transmission is not conclusive, it is widely thought that insects — flies specifically — play a central role in the spread of sarcoids with BPV detected in several common fly species. Ulcerated, bleeding lesions attract flies that may act as intermediates moving between wound sites on different horses.

“The tumors can have tendrils of cells that splay out from the main sarcoid, which are not visible to the surgeon, and that tend to react with aggressive new growth when cut. This is why surgery is generally accompanied by some form of local chemotherapy, and without this follow- up treatment, is really rolling the dice.”
— Matt Durham, DVM, DACVSMR, Platinum Performance® Technical Services Veterinarian
Diagnosis and Identification
Sarcoids can resemble other skin conditions, and laboratory analysis may be needed for an appropriate diagnosis. Biopsies of sarcoids are typically avoided since disturbance from the procedure frequently triggers the sarcoid; veterinarians usually do not perform them unless there is doubt about whether the skin lesion is a sarcoid. Biopsy is only undertaken with the understanding that a treatment plan must be initiated as soon as results are available.
It is critical to identify the type of sarcoid a horse has to insure the most appropriate treatment. Identification can be difficult as sarcoids have a range of presentations, and the diagnosis is further complicated if the animal has multiple types at once. Inappropriate or incomplete treatment can compound the tumor’s growth, making the lesions more aggressive and more difficult to treat, and lead to a recurrence.
Identifying The Six Types of Sarcoids
-
Occult
Appearance: Gray, flat and hairless areas of skin, often subtle in appearance especially in early development. The irregular skin is rough and may feel slightly thickened. Because of its circular or oval shape, occult sarcoids are often mistaken for ringworm.
Traits: These sarcoids grow very slowly and may remain static for years. However, if accidentally traumatized, they can rapidly develop into one or more serious types of sarcoids, including fibroblastic.
Found: On the nose, side of the head, neck, armpit and between the hind legs.
-
Verrucous
Appearance: Can be gray, scabby, scaly or wart-like in appearance. They may contain small, solid nodules (growths of abnormal tissue) that appear singularly but often can merge into larger, multiple lesion groups. Verrucous sarcoids extend deeper than the occult type and have a more irregular outline and uneven surface that may resemble ringworm or scarring. The skin may crack easily and scaly flakes often can be rubbed off from the surface.
Traits: Slow growing and the least aggressive sarcoid type, they are often non-painful on manipulation; however, interference may stimulate these lesions to change into a more aggressive form of sarcoid and potentially can develop into both fibroblastic and malevolent forms following inappropriate handling or treatment.
Found: Around the head, groin, sheath and armpit body regions.
-
Nodular
Appearance: Discrete, solid nodes with a spherical appearance. They may have a wide, flat base or a narrower stem-like base and can appear on their own but are often seen as well-outlined lumpy groups.
Traits: Unlike other types, nodular sarcoids are covered and firmly attached by an overlying layer of normal skin. Even with the skin coverage, they have the potential to ulcerate and bleed. Agitating these lesions can result in rapid growth and possible transformation into a more drastic type, particularly the fibroblastic form. This type of sarcoid varies in size, some being more than 5 cm (2 inches) in diameter, with a medium growth rate subject to change over time.
Found: Around the eyelids, armpits, inside thigh and groin areas.
-
Fibroblastic
Appearance: Fleshy, irregular masses — often in clusters of tumors of variable size and shape that grow rapidly — typically having wet, bloody ulcerated surfaces. Fibroblastic sarcoids can begin as round or irregular, raised, firm lumps and are usually smooth and hairless at least over part of their surface; smaller ones are sometimes covered with normal skin.
Traits: Can have a wide, flat base but after growth, or if the surface becomes damaged or compromised, such as from a skin wound, the tumor will ulcerate, bleed and appear to “hang” on a stalk (pedunculated) or become extremely invasive into the surrounding skin. They have the potential to develop at wound sites, particularly damage overlying limbs, and often take the appearance of infected granulation tissue.
Found: Anywhere on the body and have the potential to develop quickly from verrucous or nodular sarcoids.
-
Mixed
Appearance: Include a mixture of two or more types of sarcoids, often of different ages, forming a “colony.”
Traits: It is common for horses susceptible to skin tumors to display mixed characteristics and to develop multiple sarcoid types in one region or the appearance of multiple sarcoid types at different sites around the body.
Found: In any area, but they most often appear on the head, armpit and groin areas.
-
Malevolent
Appearance: Extremely rare and the most aggressive type of tumor that spreads extensively from the original site through the skin and subcutaneous tissue.
Traits: Sometimes confusingly referred to as “malignant” (because of their severity), but these tumors do not metastasize to internal organs. They can continue locally along lymph vessels producing cords of tumor tissue interspersed with nodules and secondary ulcerating fibroblastic lesions that tend to form into larger groups. Because this uncommon type can spread over a wide area and grow quickly, malevolent sarcoids can become quite difficult to manage. While some cases develop spontaneously, malevolent sarcoids can be the result of repeated incomplete or unsuccessful treatments.
Found: Most commonly affect the face, elbow and inner thigh regions.
“Sarcoids are really frustrating. I’ve never heard of so many different treatments for a disease, which usually means that none work consistently. In general, it’s always great when the immune system does most of the job.”
— Matt Durham, DVM, DACVSMR, Platinum Performance® Technical Services Veterinarian
Treatments
Historically, and still today, sarcoids are subject to “benign neglect.” They are left untreated with the hope that they will eventually heal or stay stagnant. All sarcoids should be taken seriously when first detected, and a veterinarian should assess even small ones. While it may be best to simply monitor a small sarcoid that has recently developed and is not causing interference, your veterinarian should make that decision. Early intervention is recommended and most effective when the lesions are small. Moreover, scarring is also less obvious when sarcoids are treated or removed before they enlarge. The tumors may remain unchanged for many years, but it is important to watch for any signs of change. Unfortunately, many sarcoids will eventually increase in size and become more difficult to treat, requiring more invasive therapies or a combination of treatments.
Sarcoids can be extremely challenging for veterinarians to treat as there are numerous options and none are universal to eliminate all tumor types. Compounding the dilemma is should the treatment fail, it may worsen the situation. Any interference can “wake up” and convert a simple sarcoid into a larger or more aggressive type. There is always the risk of recurrence, particularly at or near the removal site of the lesion. Recurrence typically happens within six months, and often sarcoids return more destructive than the original tumor. Once the sarcoid is identified, multiple factors will influence the treatment options. These include: type, size and number of sarcoids; location and extent of the sarcoids; treatment facilities and medications available; the horse’s temperament; as well as cost considerations. Surgical treatments include physical removal, laser surgery and cryosurgery (freezing). Immune modulation treatments may include BCG (bacillus Calmette-Guérin) injections or autologous implantations. Medical management options include chemotherapy, electrochemotherapy, radiation and topical treatments. More than one type of treatment may be used at the same time in combination depending on the sarcoids present.
It is important to have every sarcoid assessed by a veterinarian as the treatment options vary between individual sarcoid types with the goal to select the best treatment that will be the most successful the first time.
Sarcoid Treatment Options
-
Surgical Removal
Surgical removal is common and a viable option dependent on the location of the tumor. General anesthesia may be used, although local anesthetic is usually adequate, and a single or small number of sarcoids can be simply cut out. Nodular sarcoids often respond well to surgical removal. The wound can be stitched or left open to heal from the inside out forming a scab and usually resolving in four to six weeks. However, failure to remove the entire sarcoid will increase the chances of aggressive recurrence. For this reason, veterinarians usually include a wide surgical margin around the tumor. While the procedure is simple, the surgical excision failure rate is high with an over 80% recurrence rate with surgery alone, particularly without additional therapy. Cryotherapy is often used with surgical intervention and improves success rates. Benefits of surgery include a fairly quick healing time, good cosmetic results, and it can be effective in some difficult areas like the ears.
-
Laser Surgery
Laser surgery, a relatively new technique, is becoming more widely used. Where available, a laser removes the tumor as well as its base, along with a margin of healthy tissue to prevent re-growth. Because the tissues are burned, bleeding is minimal. Standing sedation is usually used with local anesthetic, or the horse may be put under general anesthetic. This treatment has success rates of over 80% and low risk, but healing and recovery can be a slow process with scar formation.
-
Cryosurgery (Cryotherapy, Freezing)
In cryosurgery, liquid nitrogen is used to rapidly freeze tissue and kill the rapidly dividing cancerous cells. This treatment is often used on small, occult-type sarcoids, and to prevent recurrence it is also used to treat the base and any remaining sarcoid tissue following a de-bulking surgery. Because hair follicles are damaged, patches of white hair usually develop at the treatment site. Cryosurgery can be time consuming, may require repeated treatments, and is not often a primary or preferred treatment option.
-
BCG Injection (Immune Therapy)
The BCG (bacillus Calmette-Guérin) injection works by local immune modulation. The BCG injection is produced from Myobacterium bovis, a bacterium actually used to immunize against tuberculosis. Essentially, BCG is directly injected into the sarcoid to stimulate the immune system and provoke a reaction to destroy or reject the tumor tissue. It is mostly used for sarcoids located near and around the eyes, especially nodular types. Multiple injections over several weeks or months are required. Heavy sedation is usually needed, and anti-inflammatory medication is given before each injection to reduce the risk of allergic reaction.
-
Autologous Implantation
Autologous vaccinations — autologous means “from the same individual” — are a common technique used to aid other livestock species. For equine sarcoids, a small sample of the tumorous tissue is taken, frozen in liquid nitrogen to kill the virus, thawed and implanted back into the horse’s body (usually the neck). The implant stimulates an immune response and uses the animal’s own immunity to recognize the tumor as foreign and attack it. Ongoing research is dedicated to this promising treatment.
-
Chemotherapy
Cisplatin and carboplatin chemotherapy drugs are injected directly into sarcoids and act by interfering with the DNA replication in tumor cells. These drugs can cause local inflammation and possible scarring. Treatment costs can be expensive and will likely require multiple doses over months dependent on the sarcoid.
-
Electrochemotherapy (ECT)
Electrochemotherapy combines the use of a chemotherapeutic (typically Cisplatin) drug with electric pulses to increase its effectiveness. High-voltage electric pulses open the cell walls allowing a significantly increased concentration of the drug to enter the cell and deliver a more potent dose. The procedure is brief, usually under 15 minutes, and requires general anesthesia. Recent studies have shown that the combination of surgical debulking of the tumor followed by ECT had very high success rates.
-
Radiation (Radiotherapy, Interstitial Brachytherapy)
Radiation has been shown to be a highly effective treatment for tumors that do not respond to traditional therapies, including lesions on the legs and around the eye. It may also be the best option for aggressive, recurrent sarcoids. This type of treatment is expensive and not widely available (usually offered at specialized hospitals), often requiring general anesthesia.
-
Topical Treatments (Imiquimod (Aldara), bloodroot extracts)
Topical treatments are used widely on sarcoids. These specific, veterinary-use only cytotoxic preparations that often contain anti-viral and anti-tumor ingredients, attack and kill abnormal tumor cells. They are often creams and can be very effective when used to treat smaller, flat occult type sarcoids, or as an adjunct treatment following the surgical debulking of larger sarcoids. Treatment time can be long, up to several months, and often the sarcoid will appear worse before it improves. Topical preparations can be painful with localized inflammation and swelling common and have the potential to damage healthy tissue. The treatments are not ideal to use on sensitive bony areas or places with concentrated nerve or blood vessels.
In Conclusion
Sarcoids are a progressive and persistent form of cancer that can develop anywhere on the skin, but commonly appear on the head, chest and groin areas. Usually locally invasive, the tumors do not spread to other organs. Sarcoids are frustrating as there are different types that behave in a number of ways and respond to a variety of treatments. Sarcoids require careful veterinary assessment to choose the most efficacious treatment for the specific outbreak.
Inappropriate treatment can exacerbate the sarcoid, making it more aggressive and more difficult to treat. If you suspect sarcoids on your horse, contact your veterinarian. The best results are achieved when a diagnosis is made and appropriate treatment occur early.
More in Our Podcast; Subscribe Today
What to Know & How to Tackle Sarcoids
From the root cause to a wide range of treatment options, challenges and recurrence rates, Dr. Matt Durham guides us in what to consider and how best to manage these frustrating tumors.
Listen