Understanding the Causes, Signs and Diagnostic Methods
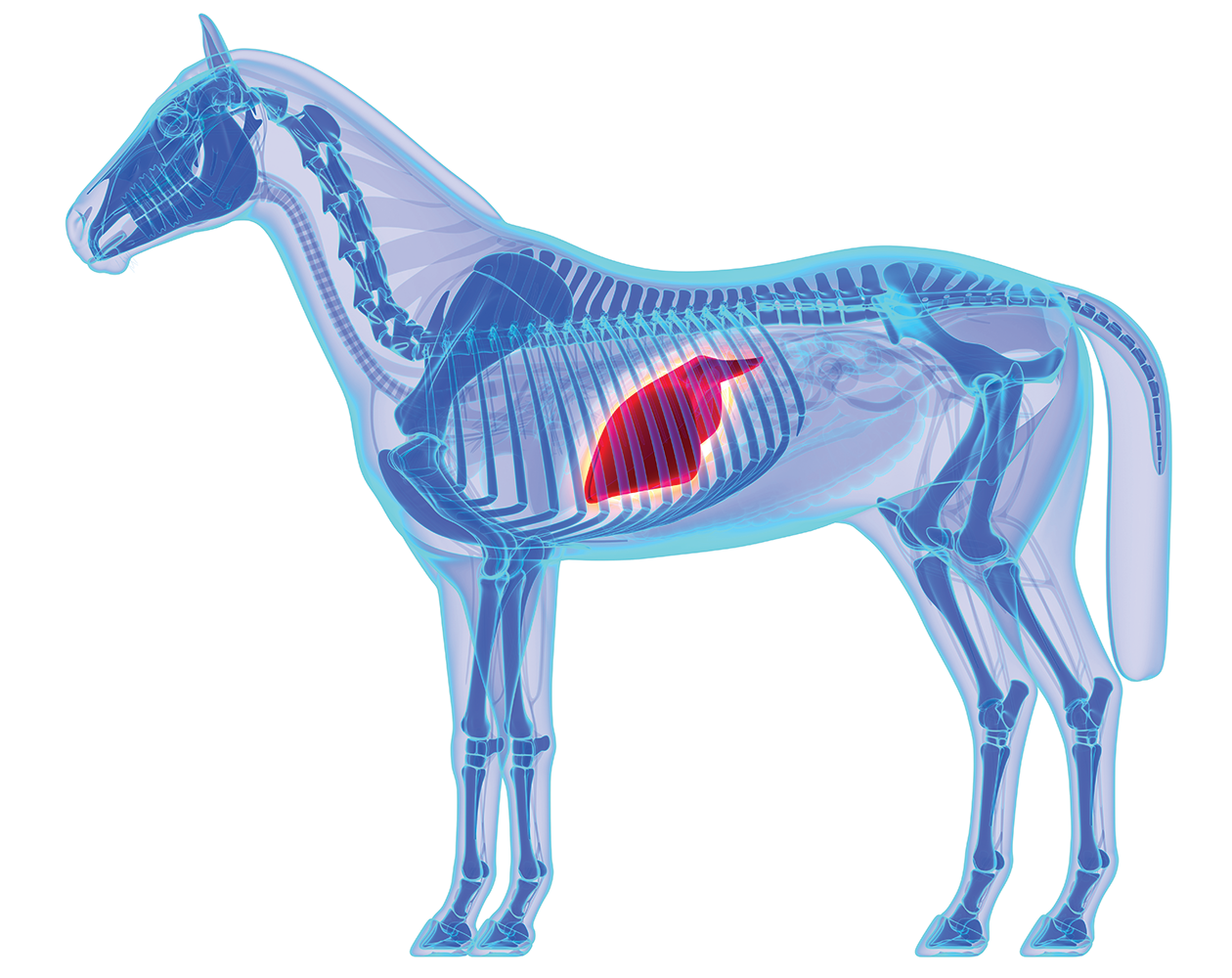
The liver in a horse has a big job and the tools to do it. It’s the largest internal organ, weighing about 11-13 pounds, or about 1.5% of the total body weight of a mature horse. Consequently, the liver plays a critical role in the animal’s overall health and well-being, performing detoxification and filtration, metabolizing carbohydrates, proteins and fats, producing bile for digestion, providing immune support and more. Yes, it’s a heavy lift, but the liver has size with capacity enough to store essential staples of energy — glycogen and triglycerides — nutrients and essential fat-soluble vitamins including A, D and E, as well as being a major repository for iron (as ferritin/hemosiderin) and copper. And if that’s not enough, it is also capable of generating new replacement liver cells, which provide some protection against other challenges because the liver is also at risk of injury — and worse.
Equine liver disease has various causes: exposure to toxins, metabolic disturbances, infections, inflammatory conditions and genetic predispositions. When the liver is damaged or diseased, the horse can display a range of common clinical signs — lethargy, weight loss, poor appetite, colic and others. The signs are subtle, easy to overlook and may resemble other equine health issues making early diagnosis and intervention difficult, albeit critical. Unfortunately, signs of liver insufficiency may not be evident until 60- 80% of the organ is nonfunctional. So, early detection and treatment greatly improve outcomes for affected animals. While some forms of disease are treatable with appropriate veterinary intervention, others may be progressive and ultimately lead to liver failure, a grave condition with a high mortality. Liver disease is not uncommon and may affect up to one in 10 horses in clinical settings and potentially higher numbers in senior or compromised horses.
The Liver: 500 Distinct Functions
Key Roles Include:
- Detoxification: Constantly filters out and neutralizes harmful substances and toxins from the bloodstream, including waste byproducts from metabolism.
- Metabolism: Regulates energy balance, stores glycogen and breaks down nutrients like fats, carbohydrates and proteins from the gastrointestinal tract.
- Digestion: Unlike other mammals, horses don’t have a gall bladder that concentrates and stores bile. Instead, the equine liver produces a continuous flow of bile into the small intestine, which aids in the digestion and absorption of fats and fat-soluble vitamins.
- Protein Synthesis: Plays a pivotal role in synthesizing various proteins, including albumin and clotting factors — essential for maintaining blood volume and proper clotting. It also produces non-essential amino acids.
- Nutrient Storage: Converts and stores nutrients including vitamins like A, D and B12, amino acids, triglycerides and minerals, such as iron.
- Immune Support: Filters out toxins from the bloodstream, produces pro-immune proteins and helps develop blood cells.
- Blood Sugar Regulation: Produces glucose from other sugars like fructose, as well as from amino acids, glycerol and the short-chain fatty acids created in the hindgut by microbial cellulose breakdown. Serves as a major storage site for glycogen, the stored form of glucose that is the body’s preferred energy source. When blood sugar drops, the liver releases glucose.
- Homeostasis: Adjusts levels of proteins, lipids and carbohydrates that enter the blood from the digestive tract to ensure consistent nutrient levels in the bloodstream.
Common & Deadly Toxins
When the liver is compromised, systemic effects can alter a horse’s overall health. The most common cause is exposure to toxins. Horses are particularly susceptible to substances that interfere with normal cell processes, disrupt metabolism, damage nerves or kill cells. Common toxins include:
- Mycotoxins: Chemical compounds produced by molds (fungi) that grow on pasture, hay and grains, especially in warm, humid and damp conditions. Moldy hay or grain containing mycotoxins, like aflatoxins (Aspergillus fungi), can lead to liver damage.
- Drugs: Overuse or inappropriate use of certain drugs can result in liver damage. These include nonsteroidal anti-inflammatory drugs (NSAIDs), which include phenylbutazone (bute) and flunixin (banamine), as well as acetaminophen, salicylates and some antifungals.
- Plants and Fungi: Specific plants such as Crotalaria species (Crotalaria spectabilis, showy rattlebox) and Amanita mushrooms can cause liver toxicity. These and other environmental hazards contain compounds that are specifically toxic to liver cells. Ragwort, a common daisy-like flowering plant, as well as fiddleneck and groundsel, containing pyrrolizidine alkaloids, are toxic and known to damage the liver.


Possible Infectious Causes of Liver Disease
- Equine Serum Hepatitis, also called serum sickness or Theiler’s disease, is a common infectious cause of acute liver failure in horses. This virus can be transmitted following exposure to a horse serum product, such as tetanus antitoxin.
- Leptospirosis is a bacterial infection caused by Leptospira species (transmitted from contaminated water or wildlife urine) that can also lead to kidney dysfunction.
- Ingestion of liver fluke parasites, large strongyles and ascarid larvae from contaminated pasture or water sources can cause chronic inflammation and liver damage.
- Liver abscesses can occasionally occur secondary to a pigeon fever bacterial infection (Corynebacterium pseudotuberculosis) weeks after the external abscess has resolved.
- Other infectious diseases associated with liver damage in horses include the viral equine herpesvirus (EHV-1) and equine hepacivirus (EqHV) and the bacterial infections cholangiohepatitis, internal strangles infections and Tyzzer’s disease (in young foals).
Liver Disease: Contributing Factors
- Metabolic Disorders: These conditions also contribute to liver dysfunction in horses. Hyperlipidemia is a metabolic issue characterized by high levels of fats (triglycerides) in the blood, resulting from the rapid breakdown of body fat. When this exceeds the liver’s capacity to process it, excess triglycerides and free fatty acids infiltrate the organ, leading to disease. Miniature horses and donkeys are particularly susceptible. Equine Metabolic Syndrome, or EMS, characterized by insulin resistance and abnormal fat metabolism, can result in fatty liver syndrome (hepatic lipidosis). The class of drugs called SGLT2 inhibitors (medications ending in “-gliflozin”) help manage insulin dysregulation but often exacerbate hyperlipidemia and potentially fatty liver disease.
- Infectious Causes: Viral, bacterial or parasitic diseases can also impact the liver. While rare, it is still a significant concern in regions where the infectious causes are endemic.
- Copper Toxicity: Horses are particularly sensitive to a copper imbalance, and both a deficiency and overload of this vital trace mineral can lead to health issues. The liver stores copper, and excessive accumulation can lead to toxicity.
- Breeds and Genes: Certain breeds, including Arabians, may have a higher genetic predisposition to chronic hepatitis or copper toxicity. Studies suggest up to 15% of Arabian horses may have some form of liver dysfunction. Ponies too show a higher rate of general liver disease, as do pregnant Quarter horse mares, who, as a group, have a higher risk of fatty liver syndrome due to the rapid weight loss occurring from late gestation to early lactation.
- Age Factor: Senior horses are more likely to develop liver issues, such as senile cirrhosis (end-stage disease, where 70-80% of liver function is lost), cancer and age-related changes that can reduce the organ’s ability to detoxify and regenerate. Treatment options for older equines are reduced ironically by the liver’s huge reserve capacity that may mask outward signs and allow damage to accumulate over many years without notice. Moreover, older animals also have longer exposure to environmental or medical toxins.
- Iron Overload: Iron is another vital trace mineral — required for oxygen transport (hemoglobin/myoglobin), energy metabolism and immune function — that is also stored in the liver. Excess iron can cause oxidative damage. This usually occurs secondary to diet management. The equine diet is inherently high in iron because pasture and hay forage naturally contains high iron levels, but horses are normally able to regulate iron absorption quite well. Chronic iron over supplementation or high-iron well water, especially in a horse with pre-existing liver issues, can be problematic.
- Inflammation: Chronic inflammation due to underlying conditions, such as infections or immune-mediated diseases, can damage liver cells over time. Diseases like chronic active hepatitis and cirrhosis can result from prolonged liver inflammation.


Ultrasonography can provide valuable insights regarding the size, shape and structure of the liver
Ultrasonography can provide valuable insights regarding the size, shape and structure of the liver
Diagnosing the Disease
Diagnosing liver disease is challenging, as many early-stage cases are subclinical. Horses may not show clear signs until the disease has progressed significantly, when signs such as jaundice, weight loss and poor appetite are noticeable. So a thorough diagnostic approach with regular blood tests and veterinary checkups is essential for early detection — especially in older animals that experience unexplained weight loss or show changes in behavior or appetite. A veterinary physical examination will look for clinical signs and if disease is suspected the medical work-up will likely involve laboratory tests, imaging and a biopsy for a definitive assessment.
Laboratory tests include screening for liver enzyme levels. Elevated levels, such as alanine aminotransferase (ALT) and aspartate aminotransferase (AST), often indicate liver cell damage. Gamma-glutamyl transferase (GGT) is also commonly used as a disease marker, particularly related to the bile ducts. Elevated bilirubin levels can confirm liver dysfunction and jaundice. Decreased albumin or total protein levels suggest impaired function, as the liver produces these proteins. And increased blood ammonia levels is another indicator of liver dysfunction. Ultrasonography can provide valuable insights regarding the size, shape and structure of the organ, even revealing signs of liver enlargement, fibrosis or abscesses.
A liver biopsy is performed with a needle-like biopsy instrument, guided by ultrasound imaging, introduced into the liver to obtain a tissue sample. This test can provide a definitive diagnosis of disease and differentiate types of damage, such as hepatitis, cirrhosis or fatty liver, as well as providing a sample for bacterial culture to help guide antibiotic treatment, if necessary.
Signs of Equine Liver Disease
The clinical signs of equine liver disease vary greatly depending on the severity and type of liver condition. In early stages, signs may be subtle and can overlap other health issues. However, as liver function deteriorates, more recognizable signs develop.
Common signs include:
- Jaundice (Icterus): One of the most noticeable signs of liver disease is a yellowing of the mucous membranes, such as the gums, skin and the whites of the eyes, due to the buildup of bilirubin, a byproduct of red blood cell breakdown.
- Anorexia (loss of appetite): Horses may show a reduced interest in food or even refuse to eat entirely.
- Weight Loss: As liver function declines, a horse may lose weight despite normal or increased food intake.
- Colic: Abdominal discomfort can cause colic-like signs, including bloating, rolling and mild pain.
- Diarrhea:
- Fever: In infectious forms of disease, a temperature may exceed 101.5 degrees Fahrenheit.
- Depression, Lethargy: Horses may appear unusually tired, sluggish or depressed.
- Edema (swelling): Fluid buildup under the skin, particularly in the limbs, bottom of the chest and abdomen.
- Abnormal Urine Color: Greenish-brown urine may result from elevated bilirubin levels in the blood.
- Bleeding: Horses may exhibit prolonged bleeding from minor cuts or bruises due to the liver’s impaired production of clotting factors.
- Photosensitization: Skin lesions that appear as severe sunburn on the white parts of their body (face and legs) due to an inability to process the chlorophyll in plants.
- Abnormal Behavior/Hepatic Encephalopathy: The liver’s inability to filter toxins and gut bacteria metabolites in the blood can affect the brain, causing behavioral changes. Horses may appear blind, have seizures, press their heads on objects and act very irregular.
Supplemental Nutrients that Support the Liver

Add These Supplements to Your Routine and Improve Your Horse’s Overall Liver Health
- Milk thistle (Silybum marianum) contains the active ingredient, silibinin, an antioxidant that offers protection. It supports normal lipid metabolism while promoting protein synthesis in hepatocytes (liver cells), important to support regeneration and repair of damaged liver tissue.
- N-acetyl cysteine provides L-cysteine, a protein precursor to glutathione, an antioxidant that protects liver cells from oxidative damage.
- Taurine, an amino acid that provides antioxidant properties, helps protect hepatocytes.
- Vitamin E is a natural antioxidant supporting cell health by preventing oxidative stress and buttressing liver function and hepatocyte health.
- Vitamin C is an antioxidant involved in many biological processes including the regeneration of other antioxidants, such as vitamin E. Seniors and horses with compromised livers may especially benefit from supplementation.
- Omega-3 fatty acids from flaxseed offer an essential fatty acid low in sugar and starch and high in soluble fiber. Omega-3 fats offer a wide array of health benefits, including supporting normal inflammatory levels.
Treating the Condition
Treatment depends on the underlying cause, severity of the disease and how early it is diagnosed. Veterinary care begins by removing exposure to liver toxins as needed with a focus on liver regeneration if possible.
Supportive care includes fluid therapy, nutritional support and rest. Horses may be dehydrated due to anorexia and fluid loss, so intravenous fluids are needed. The equine diet is supported with high-quality, easily digestible high-fiber, moderate-protein and low-fat feeds. Supplements to bolster liver function provide antioxidants, such as silymarin (milk thistle) to promote liver cell regeneration and reduce oxidative stress. Rest and reduced exercise minimize strain on the liver and promote recovery. The pharmacological arsenal may include antibiotics (to combat infection), anti-inflammatories (corticosteroids or NSAIDs) and medications to reduce ammonia production in the gastrointestinal tract.
Addressing any underlying metabolic disorder, such as EMS or hyperlipidemia, is critical and may involve dietary changes, weight management and medication to correct insulin resistance or fat metabolism. Chelation therapy targets copper toxicity to remove excess levels and prevent further damage.

With early intervention, proper treatment and ongoing management, many horses can recover and return to normal activity with equine liver disease.
With early intervention, proper treatment and ongoing management, many horses can recover and return to normal activity with equine liver disease.
Prognosis and Management
The outlook for horses with liver disease depends on the type, cause and stage of the disease. Early intervention and supportive care significantly improves the chances of recovery — particularly for reversible cases. Chronic conditions like cirrhosis or advanced liver failure, may carry a poor prognosis, however, and euthanasia may be necessary in some cases.
Managing liver disease in horses requires long-term monitoring with regular veterinary checkups, including blood tests and imaging to track the progression of the disease and adjust treatment as necessary. A forage-based diet with balanced nutrients and supplementation can support horses with the condition.
Equine liver disease is complex and potentially life-threatening. With the liver playing such a vital role in a horse's health, dysfunction can lead to systemic complications that affect multiple organ systems. Understanding the causes, signs and diagnostic methods will help ensure the well-being of affected horses. While serious liver disease can be fatal, the organ has an incredible capacity to regenerate itself. With early intervention, proper treatment and ongoing management, many horses can recover and return to normal activity.

