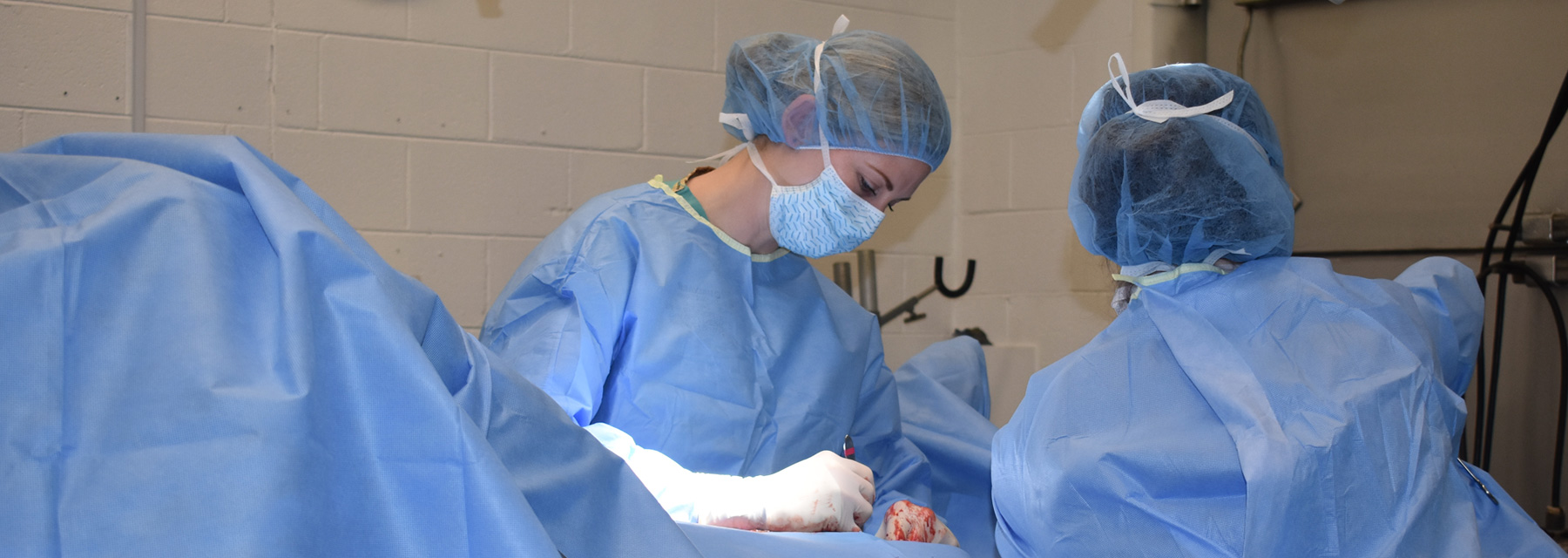
From injury prediction and prevention to treatment and rehabilitation, leading veterinarians are advancing the science of maintaining and healing tendons and ligaments in the horse.
Featuring Veterinarians Dr. Lisa Fortier, Dr. Carter Judy, Dr. Jackie Hill and Dr. Santiago Demierre
Soft tissue injuries are amongst a horse owner’s most dreaded fears and a veterinarian’s greatest challenges. Not long ago, a horse’s performance career was almost entirely lost when they sustained even a moderate soft tissue injury. An injury to the deep digital flexor tendon or suspensory ligament, for example, was career ending in many cases, rendering previously high-level equine athletes virtually unrideable.
In the last two decades, science has leapt forward, advancing the understanding and treatment of equine soft tissue injuries to a level of renewed hope. Diagnostic imaging and surgical capabilities have evolved considerably, regenerative medicine has redefined the limits of healing, nutrient therapy has given veterinarians a valuable tool to help improve patient outcomes and the science of rehabilitation has become a critical component in successfully returning horses to work post-injury.
Soft tissue injuries of the fore and hind limbs include the vital tendons and ligaments that give horses their athletic power and wide-ranging capabilities in varying disciplines. Tendons function by connecting muscle to bone while ligaments connect bone to bone, with each being imperative to performance and carrying its own challenges when injured. Along with the monumental leaps that have been made in veterinarians’ abilities to diagnose, treat and rehabilitate these injuries, there is a bright future ahead that promises a new frontier in the science of injury prediction and personalized treatment.

Diagnostic Imaging
Magnetic Resonance Imaging (MRI)
Perhaps one of the greatest factors in determining the prognosis for a soft tissue injury is in obtaining a proper diagnosis from the outset. With vast improvements in the field of diagnostic imaging, today’s veterinarians have the advantage of accurate information and a better understanding of the scope of the injury. MRI is now seen as the gold standard in diagnostic imaging related to orthopedic injuries. “MRI utilizes a strong magnetic field — 30,000 times as strong as the earth’s magnetic field — to orient the atoms of the body,” explains Dr. Carter Judy, a boarded surgeon at Alamo Pintado Equine Medical Center in California, who is widely recognized as a world leader in reading and interpreting MRI results in the horse. “By changing this field temporarily, these atoms react and emit radio waves, which are detected and interpreted by a computer to create the image,” he says. “No radiation is used, and there are no known side-effects to the use of MRI at this field strength in the horse. At Alamo Pintado, we use a high field (1.5T) Siemens Magnetom Espree. This system allows for effective, time-efficient imaging of orthopedic, soft tissue and head/ brain pathology of the horse.” The use of MRI has drastically changed veterinarians’ capabilities in terms of properly identifying, then treating soft tissue injuries in a more timely manner. “This has been a game changer for so many horses that were previously going undiagnosed for a long time,” says Dr. Jackie Hill, a boarded surgeon at Littleton Equine Medical Center in Colorado.
Ultrasound
In addition to MRI, ultrasound has been a valuable tool in both a clinic and field setting for over 30 years. Ultrasound today provides veterinarians with a highly adaptable and often portable diagnostic option ideal for capturing the longitudinal plane. “Today we have access to very handy and easily usable ultrasound machines that have improved image quality dramatically,” says Dr. Santiago Demierre, an Argentine-born veterinarian who sees a significant amount of soft tissue injury cases in practice at Palm Beach Equine Clinic in South Florida. The son of a racehorse breeder and a polo player himself, Dr. Demierre is intimately familiar with the angst owners and riders experience when their horses are diagnosed with a soft tissue injury, riding the wave of treatment and rehabilitation while hoping for the best of outcomes.
Shear Wave Elastography
While diagnostic imaging has seen exponential improvements in recent decades, the work to further its reach has continued. “There is work happening in Japan with the Japanese Racehorse Association in the area of shear wave elastography that looks very promising,” says Dr. Lisa Fortier, a boarded surgeon and highly respected researcher at the Cornell College of Veterinary Medicine. “This technology tells you the actual mechanical strength of the tissue. It is an expensive form of ultrasound commonly used to tell you the stiffness of different tissues,” she explains. “For instance, if you are ultrasounding different tissues and you have a scar, then it will be stiffer than normal, where a mineralization would be even more stiff.” While the technology is promising and used more widely in human medicine, its transition to veterinary medicine is expected to be slower due to the expensive nature of the tool.
While treating soft tissue injuries requires a multi-faceted approach, the process begins with swift and proper diagnostics. Due to advancements, such as MRI and ultrasound, and novel technologies like shear wave elastography, injured horses are now able to begin a targeted treatment regimen earlier, paving the way for greater success.
Surgical Advancements
Once an equine patient is properly diagnosed with a specific soft tissue injury, surgery becomes an option with select cases. Dr. Hill uses a variety of surgical techniques to offer patients the best opportunity for recovery, including both tenoscopy and bursoscopy. “Tenoscopy is a technique similar to arthroscopy,” she explains. “With tenoscopy, we use a small camera, but instead of viewing a joint, we are viewing a tendon sheath, which is the area filled with fluid that surrounds the tendons and ligaments. This approach allows us to take a look inside and either clean up some tears or repair things in a minimally invasive way.” In contrast, bursoscopy looks directly in a bursa, which differs from a tendon sheath because it does not completely surround the tendinous structure and is located on only one side of the tendon, between it and a bony prominence. Bursoscopy is commonly used for injuries deeper down in the foot, such as in the navicular bursa. “In this case, we again use a small camera to look into the bursa to be able to treat and diagnose those injuries more accurately,” says Dr. Hill. “There is also the needle arthroscopy, and while we don’t use it frequently, it allows us the ability to arthroscopically look in a stifle joint with an 18-gage needle,” she explains. Regardless of the surgical method chosen, the quality and capabilities of surgical equipment have given veterinary surgeons significantly greater reach in the operating room. While surgery is often a vital step in a horse’s recovery from soft tissue injury, there are numerous other options that have each played a role in improving a horse’s ability to return to work after suffering a tendon or ligament injury.
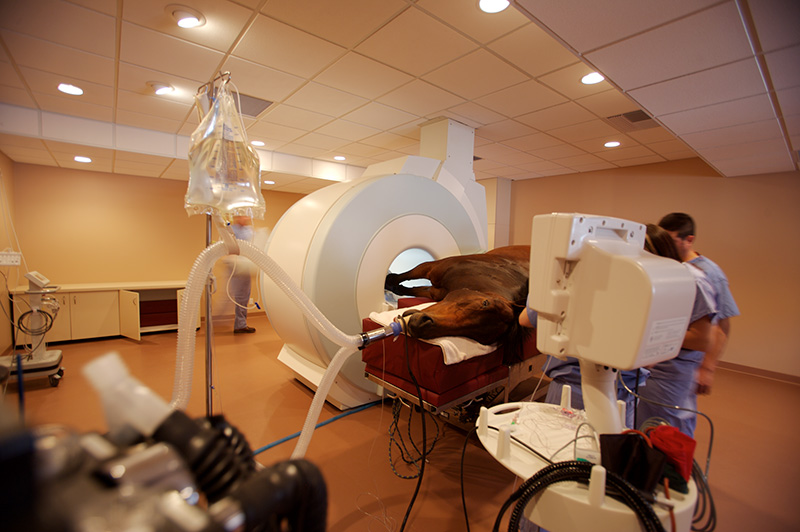

At left, Magnetic Resonance Imaging (MRI) is now seen as the gold standard in diagnostic imaging related to orthopedic injuries. Soft tissue injuries of the fore and hind limbs include the vital tendons and ligaments that give horses their athletic power and wide-ranging capabilities in varying disciplines. In the last two decades, science, including diagnostic imaging, has leapt forward and advanced the understanding and treatment of equine soft tissue injuries to a level of renewed hope. At right, Dr. Santiago Demierre, of Palm Beach Equine Clinic in South Florida, takes an X-ray of the hind, knee-joint of one of his patients.
Regenerative Medicine Furthers Healing
Stem Cells
Regenerative medicine, arguably more than any other advancement in the last several decades, has changed the shape of healing for soft tissue injury cases. The theory is simple yet profound at the same time — veterinarians use a horse’s own body to heal itself. There are generally two classifications of mesenchymal stem cells — autologous and allogeneic. Both have been widely researched, both are taken from an adult horse and not sourced from embryonic tissue, and both have distinct advantages and disadvantages. Dr. Doug Herthel, founder of both Alamo Pintado Equine Medical Center and Platinum Performance®, was an early pioneer in the use of autologous stem cells in thousands of cases beginning in 1995. The term “autologous” indicates that the cells being used to treat the horse were derived from either bone marrow or adipose (fat) tissue taken directly from that horse, with bone marrow-derived stem cells considered to be the optimal choice for potency and efficacy by many veterinarians. The second category of cells is classified as allogeneic or, in other words, cells taken from one horse, cultured, then used to treat another horse. While significant hope was placed in allogeneic stem cells for a period of time, due to the potential for these cells to be used on a broader scale as a drug, researchers and practitioners are now seeing that autologous stem cells are preferable. Autologous stem cells provide high efficacy and a lesser occurrence of side effects.
The use of stem cell therapy has only come about in the past 25 years, with veterinary medicine out-pacing human medicine in both the number and breadth of cases on which stem cell therapy has been used as a successful treatment. For many years both veterinarians and human physicians and researchers knew the efficacy of stem cell therapy but were at a bit of a loss as to how exactly stem cells behaved within the body. Why were they so effective? At first it was believed that stem cells, when placed in a tendon, for instance, would create new tendon material. Today, we know that is, in fact, not the case. “How stem cells work is through what they secrete,” explains Dr. Fortier. “They pinch off little vesicles called secretome. It’s that secretome that then provides growth factors and draws more of the local stem cells surrounding the injury into the actual injury site.” Although it sounds futuristic, there are companies that today sell secretome as a standalone treatment. To accomplish this, stem cells are grown in a laboratory setting, then the secretions from the cells’ surface are harvested, including microvesicles that are filled with growth factors and chemokines. “In this case, we don’t even need the live stem cells, we just need what the cell is producing,” explains Dr. Fortier of the secretome approach. “This gives practitioners an even clearer advantage because they will eventually be able to deliver this material patient-side. Secretome will be available like a steroid in an OTC [over-the-counter] capacity, and we won’t have to worry about immune rejection or even a bone marrow draw and the three weeks it currently takes to culture cells.”
Regenerative medicine is a bright area in both veterinary and human medicine that Dr. Fortier knows well. “Perhaps one of the most important things we have learned more recently is how to grow these cells so that we don’t incite inflammation,” says Dr. Fortier. “One of the common ways that you feed cells while growing them in a laboratory is with fetal bovine serum. We now know that the horse’s body recognizes that foreign serum and mounts an immune response. The clinical significance of that is still a bit unclear, but Dr. Ashley Watts at Texas A&M is leading the charge in discovering that we should culture these cells in either no serum at all or by using the horse’s own serum itself.”
A primary advantage of regenerative medicine is that, when paired with quick and accurate diagnosis, this type of therapy can begin immediately, interrupting the inflammatory cycle early, decreasing inflammation and intervening in the healing cascade well before the remodeling phase. This sets the stage for a more successful outcome concerning soft tissue injuries. Veterinarians at select facilities have the ability to aspirate bone marrow on the standing horse, then centrifuge it down to get “the good stuff” known as bone marrow concentrate. In more technical terms, bone marrow concentrate is the portion of the anticoagulated bone marrow sample that includes leukocytes, platelets and growth factors, among other things, with the red blood cells and other undesirable aspects separated out by the centrifuging process. Bone marrow concentrate can be re-injected to the injury site less than one hour after bone marrow was first aspirated, allowing for veterinarians to provide a near-immediate treatment option while they wait for cells to culture, a process that takes up to three weeks to accomplish for the first re-treatment. “We know that it’s critical to get to lesions early. We are already starting to fall behind if we wait and do nothing until the stem cells are cultured for re-treatments. At the minimum that animal should have corrective shoeing, proper nutritional intervention and active rehab, then perhaps some other modalities like PRP, IRAP or Shockwave, amongst others,” says Dr. Fortier.
“We know that it’s critical to get to lesions early. We are already starting to fall behind if we wait and do nothing until the stem cells are cultured for re-treatments. At the minimum that animal should have corrective shoeing, proper nutritional intervention and active rehab, then perhaps some other modalities like PRP, IRAP or Shockwave, amongst others.”
— Dr. Lisa Fortier, A Boarded Surgeon and Highly Respected Researcher at the Cornell College of Veterinary Medicine
PRP, IRAP & Pro-Stride
In contrast to re-injecting bone marrow concentrate while waiting for stem cells to culture, tools such as Platelet Rich Plasma (PRP), Pro-Stride® (Autologous Protein Solution Device) and Interleukin-1 Receptor Antagonist Protein (IRAP) can be used to attain an immediate effect as well. PRP uses a concentration of the horse’s platelets in the form of blood plasma to bring growth factors to the injury site and begin the healing process. “PRP can help decrease some of that inflammation and prevent some of the break down,” explains Dr. Hill. In contrast to PRP, IRAP is generally specific to joints, though some veterinarians rely on this treatment for inflamed suspensory ligaments. IRAP begins with a horse’s own blood, which is then incubated with specific glass beads to increase the amount of naturally occurring IRAP present. The mixture is then administered by an intra-articular injection with the goal of blocking interleukin-1, a major inflammatory component released by the body in the event of an injury. “IRAP is mainly an anti-inflammatory for the joint but also has some other important factors and components. I have seen IRAP be very beneficial for some horses with a mild cartilage injury as well, and it’s a better option than using steroids for long-term healing,” says Dr. Hill. In addition to PRP and IRAP is a device that produces a combination of the benefits of both therapies. Pro-Stride® is a proprietary dual-device system that begins with the horse’s own blood and within 20 minutes is able to produce a concentrated solution of cells, platelets, growth factors and anti-inflammatory proteins (including IRAP) that is then administered by intra-articular injection. Interestingly, bone marrow concentrate also contains very high concentrations of IRAP.
Horse owners and veterinarians are often left to decide the best course of treatment, choosing between stem cell therapy, PRP, Pro-Stride® and IRAP based off of the horse’s individual case, severity of the injury and financial considerations of each treatment option. “From a purely medical standpoint, stem cells have been shown to have the best ability to both enhance healing and reduce inflammation. They would be my first choice,” says Dr. Hill. “At the same time, stem cells are a larger financial investment for the owner, and practically, that has to be taken into consideration. This is where things like PRP come in as a viable option. My optimal recommendation when I see a horse with a new tear in a suspensory or superficial digital flexor tendon is to immediately put PRP in there, then collect bone marrow and culture cells to inject a few weeks down the road.”
“We know that with both the deep soft tissue injuries and arthritis there is a large inflammatory component — an immune-mediated inflammatory component. We often think of them as purely degenerative diseases, but they aren’t simply degenerative. There is a very important immune system contribution, especially in the early phases.”
— Dr. Lisa Fortier, A Boarded Surgeon and Highly Respected Researcher at the Cornell College of Veterinary Medicine
The Role of Inflammation and Oxidative Stress
Inflammation and oxidative stress not only play a vital role in the healing process concerning soft tissue injuries, but perhaps of greater importance, they can increase a horse’s risk of injury in the first place. A horse in a managed state of inflammation will be more capable of handling minor insults to the tendons and ligaments without becoming clinical. In contrast, a horse in an unmanaged state of inflammation will be predisposed to both soft tissue injury and joint disease, such as arthritis. A horse’s level of inflammation can be influenced by several factors, including its environment and training, but diet has been shown to be amongst the greatest determinants of whether a horse’s inflammation is kept at a managed, healthy level or goes unchecked.
Much like inflammation, a horse’s level of oxidative stress can make them more prone to injury and disease. Oxidative stress is a direct cause of cellular aging and is the body’s response to excessive free radical damage, which can be the result of rigorous training, environmental pollutants and a diet high in rancid fats and feeds. “Like in every aspect of life, everything is about balance,” says Dr. Demierre. “Inflammation and oxidative stress are responses from the body and, in certain amounts and for short periods of time, they can even be beneficial for the normal function of the body’s biological systems. When unregulated, however, they can, and usually do, become detrimental.” Dr. Fortier agrees, “We know that with both the deep soft tissue injuries and arthritis there is a large inflammatory component — an immune-mediated inflammatory component. We often think of them as purely degenerative diseases, but they aren’t simply degenerative; there is a very important immune system contribution, especially in the early phases. There’s a large portion of T cells and macrophages that are involved in the propagation of disease whether it’s an early tendon injury or arthritis,” she explains. “Understanding what’s happening in the very beginning allows us to create windows of opportunity for therapeutic intervention. One of the biggest things that we are finally starting to appreciate is that we have to treat these injuries early before scar tissue is set up.”
While inflammation and oxidative stress may play a significant role in a horse’s risk for both injury and disease, they are factors that can be prevented and also treated with the right intervention. Diet, therapeutic nutrition, proper conditioning and aggressive and early treatment after injury can all influence a horse’s inflammatory state, chance of injury, rate of recovery and risk of re-injury.
Changing Outcomes with Rehabilitation
Undoubtedly one of the most significant factors in successfully treating soft tissue injuries, aside from regenerative therapies, is the exponential gains seen in the science of rehabilitation. Veterinary-directed rehabilitation has surged forward in recent years with the advent of new technology and techniques, as well as the founding of the American College of Veterinary Sports Medicine and Rehabilitation. Veterinarians and surgeons alike were previously frustrated that they would treat a horse or operate on a soft tissue injury only to send the horse home to be confined to a stall with no active rehabilitation plan. This approach differed greatly from human medicine, where physical therapy is a mainstay in the recovery process. “We don’t just stick horses in box stalls for 4 to 6 months anymore,” says Dr. Fortier. Rehabilitation and active rehab go so much further than simply controlled forms of exercise, but now include extremely effective modalities and a solid place for therapeutic nutrition. “Modalities like Shockwave therapy, laser therapy, therapeutic nutrition, proper farrier application and regenerative medicine are all key components,” says Dr. Fortier. “All of these things combined have increased our chances of not only getting the horse back to performance but sustaining performance. I tell my clients that they have to be committed to the rehab. It’s a least half of the equation in terms of the horse’s chance of recovery.”



Veterinary-directed rehabilitation has surged forward in recent years with the advent of new technology and techniques, as well as the founding of the American College of Veterinary Sports Medicine and Rehabilitation.
A Preventative Approach
Though diagnostic imaging, surgical capabilities and rehabilitation have all improved greatly over the last two decades, veterinarians’ primary goal is to proactively prevent soft tissue injuries rather than reactively treating them. Dr. Demierre sees primarily high-level sport horses and believes in a simple but profoundly effective strategy in preventing injury. “There are four critical points I focus on,” he says. “First is proper conditioning and not working a horse to the point of fatigue. This often brings negative consequences. Second is optimum nutrition. Horses, especially athletes, need a complete and balanced diet according to their discipline and workload. Third is proper footing, avoiding working horses on ground that is too soft or too hard. Lastly, I encourage riders and grooms to use their hands and learn how to palpate the legs as part of their daily routine.” While the approach may sound surprisingly simple, veterinarians see a significant amount of cases that have sustained a preventable soft tissue injury. A whole-horse approach is imperative to shaping more durable athletes that are well prepared for their workload and have the tools necessary for greater longevity and sustained performance. Several key factors can make the difference between a high-performing, healthy animal, and a horse prone to injury. Managing a horse’s level of inflammation through diet and simple, targeted supplementation is an integral piece of the care plan, as well as monitoring body condition to maintain an ideal weight for the horse’s health rather than the discipline’s desired aesthetic. In addition, conditioning the horse appropriately for their level of performance is imperative. “It’s so important for training to be personalized and consistent and to realize that we can’t keep horses in a stall all week, then expect them to go out on a 20-mile trail ride on the weekend without injury,” says Dr. Hill. “I am a big fan of horses being turned out and having active rest periods as opposed to constantly being in a stall.” Conditioning horses correctly can help ensure that their muscles are adequately prepared for both their training and showing workload. This attention to detail also helps to avoid the fatigue that can often leave horses at a greater risk for injury.
While many riders think of conditioning as applying to their competitive horses, in fact, the process starts with foals and should remain a mainstay throughout a horse’s life and performance career. This is of particular importance as young horses are started and brought up through the ranks of training and competition. “Many horses are started very young and are trained more aggressively than their body is able to handle at that point in their life,” says Dr. Hill. With horses not reaching skeletal maturity until the age of five, these young athletes are often overstressed and left vulnerable to injury. Dr. Demierre insists it starts with the foal, and that nutrition is the first step in the conditioning process. “Provide the foal with proper nutrition, especially during the first two years of life when musculoskeletal development is at its apogee,” he advises. “It’s important not to rush things and give the horse time at every step of the training process, especially during the first two years of work under saddle.”

The world of therapeutic nutrition has seen substantial advancements in recent decades. A whole-horse approach is imperative to shaping more durable athletes that are well prepared for their workload and have the tools necessary for greater longevity and sustained performance. Dr. Natalie Zdimal, above, talks with Platinum Performance® client Kristen Hiller.
“I absolutely think it plays a role in the healing stage of injuries, but more so, the best use for therapeutic nutrition is in the preventative stage.”
— Dr. Jackie Hill, A Boarded Surgeon at Littleton Equine Medical Center in Colorado
The Impact of Therapeutic Nutrients
The world of therapeutic nutrition has seen substantial advancements in recent decades, giving veterinarians and riders a tool to impact not only the healing process post-injury but to help prevent soft tissue injuries by targeting the inflammatory process and, more specifically, joints, tendons and ligaments locally. “As veterinarians, we can sometimes get caught up in the big picture and forget that we could get our patients recovering faster if we didn’t leave out the nutritional side of things,” says Dr. Hill. “I absolutely think it plays a role in the healing stage of injuries, but more so, the best use for therapeutic nutrition is in the preventative stage.” True prevention comes with approaching tendon and ligament health by way of the horse as a whole and appreciating that a horse in an unchecked state of inflammation will be more prone to injury and disease. “Inflammation is subtle at a microscopic level. When we don’t realize that, we’re missing all of those early inflammatory stages until we get to the point of ‘Oh no, we already have disease,’ ” points out Dr. Fortier. “By the time the horse has a limp or pain on palpation, you're already well into the disease process — you’re not just dealing with inflammation anymore. If you are not on some type of preventive, then you’re probably at a greater risk for tendon and joint injury.”
Convincing research is ever-evolving, showing that omega-3 fatty acids are a weapon in the armory of tools used to fight inflammation. The horse relies entirely on its diet to obtain the necessary omega-3 fatty acids it requires. Where the horse was once a roaming grazer, consuming ample omega-3s from grasses, various foliage, flowers and barks, equine athletes today are significantly more confined and fed one to three daily meals instead. With domestication, the horse’s diet also transformed from pasture grasses to a mix of hays, grains and concentrates. Hays are grown today on largely mineral-depleted soil and lack the vital omega-3s and crucial antioxidants that help keep a horse’s systemic level of inflammation at a healthy level. Past that, grains and processed concentrates can deliver a high peroxide level due to the high-heat, high-moisture and high-pressure environment necessary to produce most pelleted feeds. By returning to a more natural diet of high-quality forage, supported by simple and targeted nutrient formulas, equine athletes are returning to what their bodies were designed to process and use most efficiently. “Omega-3 fatty acids are the most convincing across the board, not just related to soft tissue injury but to cellular aging in general,” says Dr. Fortier. “There is clear evidence that omega-3 fatty acids are excellent for the benefit of the whole horse. I recommend Platinum Performance ® CJ because it has the omega-3s and antioxidants in there as well as the ingredients that support the joints and soft tissue. I’m an orthopedist, so of course those specific ingredients are what I need, but I choose it because of its combinational approach.”
It’s that combinational approach that allows veterinarians and riders the ability to target joints and soft tissue while concurrently providing the horse with the core omega-3 fatty acids and antioxidants that are imperative for overall health and performance. In addition to those core nutrients, vitamins and minerals, there are key therapeutics that target joints, tendons, ligaments and cartilage specifically. ASU, or avocado/soy unsaponifiables, are derived from the lipid portion of avocados and soy, and have been shown to help support cartilage synthesis and aid the body’s natural ability to fight articular cartilage breakdown. Hyaluronic acid, known as HA, is a non-sulfated glycosaminoglycan that is naturally found in connective, epithelial and neural tissues. HA is a major component of synovial fluid, which surrounds joints and supports normal mobility between articular cartilage that can occur during movement. Certain oral hyaluronic acid sources have been shown to be highly bioavailable, or absorbable, and are an excellent tool to help support joints and soft tissue. Other beneficial ingredients are cetyl-myristoleate, which helps the body to support normal levels of inflammation, while supporting chondrocyte production, as well as MSM, or methylsulfonylmethane, which provides a bioavailable sulfur source that is a key component in most glycosaminoglycans, cartilage, tendons and ligaments. Another key component to supporting post-injury soft tissue healing is incorporating silicon into the horse’s regimen. One of the most abundant elements on earth, silicon is required for the formation of tendons, ligaments, cartilage and bone. Research has shown that bioavailable sources of silicon, such as the zeolite in Osteon®, support soft tissues as well as proper bone formation and calcification.
“I recommend Platinum Performance® CJ for the vitamins, minerals, omega-3 fatty acids and antioxidants but most importantly for the ASU component. During the recovery period, I think it is important that the body has all the nutrients available to try to get that joint back to a healthy state as soon as possible,” says Dr. Hill of her post-surgical recommendation. “The vitamins and minerals play a bigger role in the healing process than we realize. Providing the proper nutrition like the omega-3 fatty acids and targeting that inflammation can only be beneficial for healing and the whole horse in general.”
“My greatest pleasure is spending my time in close contact with these magnificent animals.”
— Dr. Santiago Demierre, Palm Beach Equine Clinic in South Florida
The Future is Predictive
The understanding and ability to both prevent and treat soft tissue injuries may have taken significant leaps of late, but perhaps the most substantial discoveries are still ahead of us. Veterinarians and researchers are focused on developing more targeted therapies to further improve the prognosis for tendon and ligament injuries. But, what if practitioners were able to see those injuries coming before they occurred? It turns out, they can. The science of predictive medicine, while seeming otherworldly, is actually happening now. Tools such as predictive biomarkers are being developed with the mission to give veterinarians clear and measurable indicators to predict which horses are most likely to sustain specific injuries or suffer from certain diseases. “Biomarkers could be the way of the future in terms of what leads to more personalized medicine,” says Dr. Fortier excitedly. In addition to their ability to essentially predict injury, biomarkers could allow practitioners to tailor a more personalized approach to treatment by having an inside look at what therapies will have a greater chance of success with each individual patient. “The question is how do we find out what is going to work? If we have a biomarker, then you can see that, yes, this works for this horse and, no, this doesn’t. If you have a biomarker for joint degeneration and we put PRP into the joint together with recommending therapeutic nutrition, we can see if we are going in the right direction and changing the course of the disease.” Dr. Demierre shares this enthusiasm for the potential impact that predictive medicine could have on reshaping the way veterinarians and human physicians practice medicine. “Simply put, this is a way of finding markers of a certain disease or injury in the patient before the disease or injury becomes clinical,” he says. “There are different stages in the pathogenesis of a disease with the clinical manifestation of that disease being the end stage. The idea of this new area of research is to focus on those preclinical markers in order to prevent the clinical manifestation of the disease from ever occurring. This will likely be a powerful tool.”
Though further research lies ahead to solidify this emerging science, biomarkers appear to be setting the stage for a new frontier in medicine. No longer will we take general steps to prevent injury and disease, we could instead be armed with specifics unique to each patient. The potential is vast and just years from now we could see a dramatic decrease in sports-related injuries, disease occurrence and onesize- fits-all therapies. The future is predictive, it’s personalized and hopefully, it’ll be here within the not-too-distant future.
Redefining Limits
The research and in-practice work that has been done in the realm of soft tissue injuries has truly reshaped a vital aspect of veterinary medicine and equestrian sport. Just two decades ago, a horse’s chance of returning to work after a tendon or ligament injury was just 20 percent. Today, with tools such as advanced diagnostic imaging, surgery, veterinary- directed rehabilitation, regenerative medicine and therapeutic nutrition, that number has climbed as high as 80 percent. To the veterinarians whose lives are dedicated to treating equine athletes, it’s not simply the achievements of modern medicine that have them celebrating this shift. It all comes back to the love of the horse and their ability to help change the trajectory of their patients’ futures. “My greatest pleasure is spending my time in close contact with these magnificent animals,” says Dr. Demierre sincerely. “Personally, the best feeling is when I see the results of all of my efforts paying off and we have a successful outcome.” It’s that same motivation that keeps Dr. Hill and her friend, colleague and mentor, Dr. Fortier, firmly pointed toward further improvements in their craft. “I have loved horses as long as I can remember,” says Dr. Fortier. “In the end, it’s all about them,” agrees Dr. Hill. “It’s about getting some little girl’s horse working again or just having the chance to improve the quality of a horse’s life. We love the science, yes, but we do this because we love the horses and we want to see the best for them.”




From the left to right: Dr. Lisa Fortier, a boarded surgeon and highly respected researcher at the Cornell College of Veterinary Medicine (photo by Scott E. Palmer, VMD); Dr. Carter Judy, a boarded surgeon at Alamo Pintado Equine Medical Center in California, who is widely recognized as a world leader in reading and interpreting MRI results in the horse; Dr. Santiago Demierre, an Argentine-born veterinarian who sees a significant amount of soft tissue injury cases in practice at Palm Beach Equine Clinic in South Florida; and Dr. Jackie Hill, a boarded surgeon at Littleton Equine Medical Center in Colorado.

by Jessie Bengoa,
Platinum Performance®
You May Also Like

Managing Common Muscle Disorders in Horses
Management procedures and specific dietary interventions can help reduce the severity and the frequency of episodes.
Read More about Managing Common Muscle Disorders in Horses
The Science of Sport
The Evolution of How We Treat, Condition & Feed the Competitive Athlete.
Read More