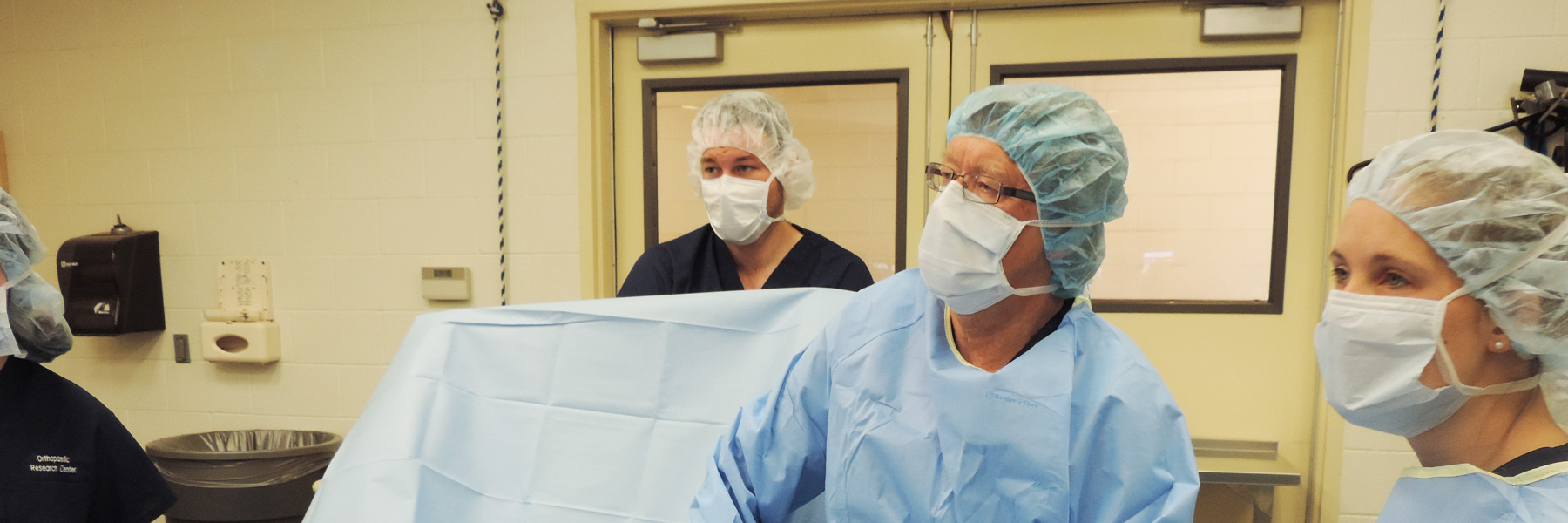
Insights by Masters in the Field, Doctors Wayne McIlwraith & Larry Bramlage
"It's been estimated that 60% of athletic horses are retired because of osteoarthritis." This is a staggering statistic, particularly coming from Dr. Wayne McIlwraith, a man that has spent nearly every waking moment of his professional career improving the understanding and treatment of such a prolific condition as osteoarthritis (OA). Dr. McIlwraith's life’s work has been charted within the confines of equine joints. He and fellow veterinarian, surgeon and researcher Dr. Larry Bramlage are world renowned authorities in the study of osteoarthritis and have made tremendous strides in the use of arthroscopy in joint therapy over the last four decades. They also have had a hand in a remarkable number of major discoveries centered on the treatment of equine joint disease, from early research on the role of inflammation in joint degradation, to the future of biologic therapies.
Pathways to Discovery
It’s hard to imagine McIlwraith and Bramlage, two undeniable greats, as green veterinarians just breaking into the field. However, their tenacity foreshadowed the great accomplishments they’d achieve. “I graduated from vet school in New Zealand, and I certainly hadn’t heard of arthroscopy. But I don’t think anybody had,” says McIlwraith. “It just wasn’t being used back then.” It was the mid 1970s, and like McIlwraith, Bramlage was at the beginning of what would become a storied career, having graduated from veterinary school, then completed an internship at Colorado State University and moved on to a residency at Ohio State while McIlwraith completed an internship at the University of Guelph and moved on to a residency at Purdue. “I stumbled into arthroscopy when I was a resident spending time at human hospitals,” remembers Bramlage. “The arthroscope was just coming on the scene. It was 1977, and that was before we as surgeons were the primary treatment for most joint diseases. Surgery was more of a last resort then, and the arthroscope was just starting to be used to diagnose meniscal problems in the human knee.”
As it turned out, a connection with human medicine would lead both McIlwraith and Bramlage down the path of arthroscopy, taking what was a novel human orthopedic tool and carrying it to new heights in veterinary medicine. “I had a client in the late 1970s who had hunters,” remembers Bramlage. “Her husband happened to be an orthopedic surgeon who was one of the early people interested in arthroscopy. He invited me to a human arthroscopy course, held in Cincinnati, Ohio, in 1981, and I was the only veterinarian there. The study of arthroscopy at that time was centered on how to insert the arthroscope, then find the probe. When compared to even basic modern arthroscopy courses, it was very rudimentary.”
Similarly, McIlwraith’s first glimpse at the human orthopedic applications of arthroscopy ignited an epiphany of sorts, “I went to a course in human arthroscopy in 1976 with Dr. Lenny Johnson at Michigan State University Medical School, and I thought it would have a lot of use in horses,” he remembers. “The course was just 100 physicians, orthopedic surgeons and me learning how to do a diagnostic arthroscopy in the human knee.” It was that experience that convinced him of the equine applications of arthroscopy and inspired him to take a still-developing human therapy and translate it to equine surgery. As Bramlage puts it, “arthroscopy was still somewhat of a toy and not yet a clinically useful tool.”
When McIlwraith moved to Purdue University as a surgery resident, he combined his evolving interest in early arthroscopy with a research study on joint degradation. This study sparked his interest in an area that subsequently has helped shape many of the therapies and techniques used by equine orthopedic surgeons today and provided the basis for therapies that will be used in the future. “We did a study while I was a resident where we looked at synovial inflammation of the joint,” says McIlwraith, “and we showed that inflammation alone would cause early cartilage degeneration and osteoarthritis.” It may sound obvious now, but then there was little known about the primary causes of joint disease. While the causes were not yet well understood, treatment options remained almost entirely medical, revolving around systemic non-steroidals — mainly phenylbutazone — and also intraarticular corticosteroids.
“We had to intervene early enough where we could prevent the degeneration of the joint. That took a 20-year education process of ourselves, referring veterinarians, trainers and owners. And now it’s understood that the earlier you get to the joint, the better your results.”
— Dr. Larry Bramlage, World Renowned Authority in the Study of Osteoarthritis
Early Research
“People see the discovery of penicillin and think that’s the way research happens and progress is made, with one monumental discovery,” says Bramlage. “In reality, that’s not what happens. It’s a gradually accumulated body of facts that leads to the understanding of what you can and can’t do.” This was certainly the case in the study of equine joint disease and arthroscopy specifically. Small steps forward coupled with a few noteworthy discoveries combined to improve our understanding of the equine joint in the early 1980s. “The initial concept that we had to grasp was that you could not treat arthritis very effectively using arthroscopy,” continues Bramlage. “Arthroscopy is a prevention. What it does is negate the ill effects of the various insults to the joint, whether they be OCD fragments, chip fractures, even infection. Your job is to eliminate those from the joint and preserve the articular cartilage that is there.”
Initial studies performed by Bramlage at Ohio State and McIlwraith at Colorado State University (CSU) on the response of the joint surface to various treatments resulted in a stunning conclusion. “I was amazed at how ineffective almost everything was,” says Bramlage. “We had to get to the point where we understood that the whole goal was to preserve whatever cartilage you have left that’s separate from the injury. What was lost is lost, and that’s why there’s a finite limit to arthroscopy as a treatment. There’s only so much of the joint surface that you can give up without having significant detrimental effects.” Understanding both the potential and limitations of arthroscopy has brought it to the place where we know it today, as the first line of defense for most joint injuries, rather than the last resort. “We had to learn that there were many joint problems that we couldn’t solve with the arthroscope,” says Bramlage. “We had to intervene early enough where we could prevent the degeneration of the joint. That took a 20-year education process of ourselves, referring veterinarians, trainers and owners. And now it’s understood that the earlier you get to the joint, the better your results.”
Corticosteroids
Just as arthroscopy was becoming more commonplace, equine joint therapies began to expand and corticosteroids became a treatment of choice for horses with inflammation in the joint. “They were like magic,” remembers Bramlage. However, it was soon discovered that corticosteroids could have a detrimental effect when not used sparingly. “There was a rebound effect where the joints just fell apart after you’d use them,” says Bramlage. “They were wonderful initially, but it didn’t take long to pay the price for what we were doing.” The Orthopaedic Research Center at CSU (of which Dr. McIlwraith is the founding Director) had done three studies looking into the use of corticosteroids in equine joint therapy, while Bramlage and his team at Rood and Riddle were validating and stimulating further research with the large number of clinical surgeries they performed. “Through it all we began to understand that the use of corticosteroids wasn’t bad,” says Bramlage. “It was how we were using them. Corticosteroids are most easily understood with the premise that they stop everything — they stop the inflammation, they stop the pain, but they also stop all of the joint’s own ability to protect itself. That’s a viable trade-off if you’re in the process of solving the primary problem while you stop the inflammation. If you just use it to cover up the inflammation and train on while leaving the chip fractures in place, then you’re going to pay the price.”
Inflammation
McIlwraith’s early research into the effects of inflammation on the joint completely changed his view of joint disease. “Everything we knew, and it wasn’t much, had been extrapolated from human research,” remembers McIlwraith. “People would talk about osteoarthritis and claim it wasn’t an inflammatory process or that inflammation was not a primary event. What we showed is that you didn’t have to have instability, you didn’t have to have a fracture, if you just produced inflammation, then the cartilage could lose its proteoglycans, then its collagen and start undergoing morphologic degeneration. That was quite revolutionary, and one of the few instances where we were ahead of the human joint disease research.”
With a basic understanding of the role of inflammation in equine joint disease, it became important to ascertain the level of damage in clinical cases and to differentiate between inflammation caused by normal wear and tear affecting the synovial membrane or more serious damage caused by inflammation. “Inflammation is secondary to cyclic trauma, and the athletic horse is doing a lot of cycles at advanced gates. Using the racehorse as an example, you get day-to-day cyclic trauma. Not anything that’s excessive, but it can be enough to cause problems,” says McIlwraith. “The other level is when you have major soft tissue injury like a cutting horse can have,” he continues. “These horses exert tremendous stress on their hocks and stifles and can tear a meniscus, meniscal ligament or a cruciate ligament. In those cases, they have structural damage to those ligaments that then results in inflammation from the things that release from the tear. In other words, you’ve got a gradation of synovitis with varying severity of structural damage.”

Dr. Larry Bramlage, DVM, MS, DACVS, of Rood and Riddle Equine Hospital in Lexington, Kentucky.

Dr. Wayne McIlwraith, BVSc, PhD, DSc, FRCVS, DACVS, DACVSMR, of the Colorado State University Orthopaedic Research Center in Fort Collins, Colorado, and wife Dr. Nancy Goodman McIlwraith.
Stem Cells
One of the first applications of bone marrow and cultured stem cells used in clinical practice occurred in 1995. With early success in the treatment of joint inflammation and new hope for recovery from soft tissue injury, the potential of regenerative medicine ignited a fervor in the research community. “Right now, we’re at the point with stem cells where we were with the arthroscope in the late 1980s,” says Bramlage. “We know that they’re good but we haven’t scratched the surface of figuring out the best way to use them.” Significant success has been seen with the ability of cultured stem cells to return horses to work, more so than with perhaps any other treatment. “Regenerative therapies are allowing us to have horses come back from injury and compete athletically where they previously couldn’t,” says McIlwraith. “We’re using the horse’s own cells to heal itself.”
With nearly 20 years of research and clinical success with the use of stem cells, stem cell therapy is even now considered to be in infancy. The potential is limitless, with tremendous hope for the future focused on the ability to not only better understand stem cells but to control them — place a virtual target on the problem area, then send them to work. “How we use them now is that we put them into a problem, and we allow the problem to dictate how the stem cells behave, which is very effective,” states Bramlage. “There are very few things that come along that have a lot of magic to them and, to me, stem cells are the best in my lifetime. They’re absolutely phenomenal,” he says emphatically. “The trouble is, we don’t know enough about them where we can guide what they do. We’re left to a situation where we use them in areas where they logically make sense for treatment and where we allow the local environment to guide them. Many times that works, but sometimes it doesn’t and we don’t know why.”
Bramlage is convinced that once the code is broken that will allow stem cells to become a guided treatment, the possibilities will be wide open in not just equine medicine but for human patients as well. “Once someone figures out how to guide stem cells to do what you want them to do, the first target will be Diabetes,” he says. “That’s the number one healthcare problem in people, and it’s a relatively simple job for stem cells to be put into the abdominal cavity — you don’t have to create any vessels or mechanics like we do when we’re trying to recreate a joint. If you could guide stem cells to be island cells of the pancreas, then you could put them in the peritoneal cavity and they could produce the insulin for the body as a whole.” It’s a monumental possibility that stands to impact the daily lives of millions, with progress led in many instances by the past two decades of experimentation in equine medicine. “Stem cells in my mind are the key biologic therapy,” says Bramlage. “We’ve tried PRP and other therapies, and they’re a weak sister to stem cells. You can get PRP and put it into a tendon or a ligament, and it will create scar tissue and fill in that hole. But, in general, it fills it in with tissue that’s inferior. If you put stem cells in there, they’ll fill it in with tissue that’s functional much of the time.” “Actually, we have done two studies in horses demonstrating that we get enhancement of repair of articular cartilage defects merely by administering intraarticularly and in the same fashion we have decreased OA as well as showing enhanced meniscus repair in clinical stifle injury,” said McIlwraith.
Therapeutic Nutrients
Part of the biologic approach to healing, therapeutic nutrients have played an important role in helping to maintain a healthy equine joint, particularly in athletes experiencing chronic wear and tear and repetitive force from high performance. “Nutrition has been another big area of advancement when it comes to the equine joint,” says McIlwraith. “Nutrition is a component of recovery — it’s a mixture of what we know and what we think. It has become quite useful post operatively.”
Omega-3 fatty acids are one of the most extensively researched nutrients in horses, having been shown to support normal levels of inflammation in the horse and, more specifically, the equine joint. “Omega-3 fatty acids have been shown to maintain normal aggrecanase activity, and aggrecanase is the big enzyme that causes breakdown of the proteoglycans and glycosaminoglycans, which are an important component to the cartilage.” says McIlwraith.
In equine athletes, therapeutic nutrients support active joints that undergo the frequent stress of training, hauling and competition. “We use them as nursemaids,” says Bramlage. “They help support joints that are undergoing high level wear and tear, and joints that have had previous insults. I tell a lot of our clients their horse should stay on a nutraceutical for the rest of his life, as should many of us that are over 50,” he says laughing.
It’s often forgotten that providing therapeutic nutrients to horses only after they’re undergoing intense training may only be half the battle. “Nutritional management is critical for these horses when they’re young,” says McIlwraith. Indeed, starting with a solid foundation helps to maintain a healthy and well-functioning athlete from the start. And as far as McIlwraith is concerned, “there is good rational for using these nutrients.”
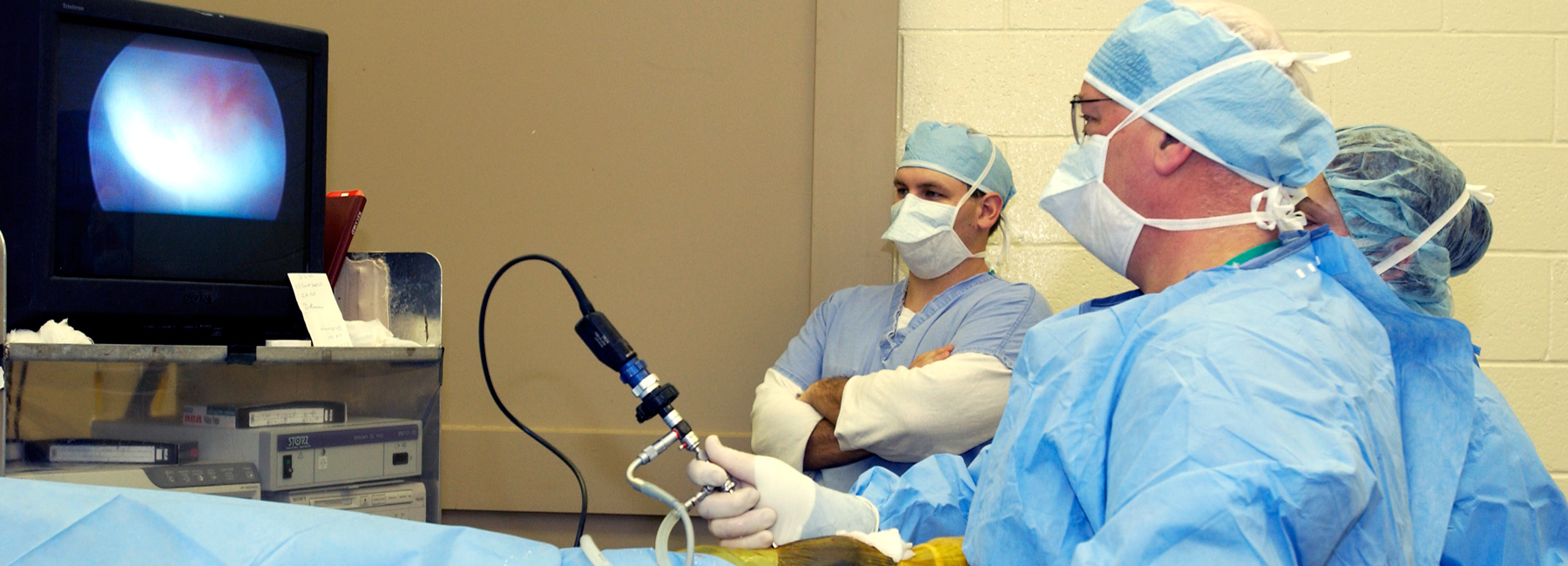
Dr. Larry Bramlage and colleagues in surgery at Rood and Riddle Equine Hospital in Lexington, Kentucky.
Training
Ask any veterinarian and they’ll tell you that the most critical care a horse receives is not after they come through the clinic gates. It starts at home, in training and day to day. A longtime fan of the racehorse, Bramlage treats hundreds of the animals each year. He knows them well and has developed a philosophy over his career that separates those horses with long-term health and success, from those without. “If you’re training racehorses, for example, you have to understand what training does to the bone and how much that horse has to build his skeleton in order to become a racehorse. Racehorse skeletons are actually molded to the work that the horse does,” he says decisively. “Trainers that understand the fact that it’s a dynamic process do very well.”
More than their training methodology, it all comes down to the willingness of the horse to accept training, retain it, then carry it into the show ring or onto the track and excel. “If you ask me what all good trainers have in common and what all average trainers could do better, I would say that the trainers who are able to read and understand a happy horse are always better,” says Bramlage. “Horses that are doing well in their work — they’re happy and they like to work. You can’t hardly keep them from going out and doing what they love to do. When a horse comes to resent training in any fashion, in any discipline, there’s something going on. The mistake that people make is not understanding that horses may not be able to talk, but their attitude shows us how they feel about what they’re doing.”
Translational Medicine
The progress being made in the pursuit of more advanced and effective equine joint therapies will see exponential benefits for the horse. Therapies are evolving, with researchers reaching high and applications being tested, improved upon and perfected in clinical practice constantly. Dr. McIlwraith and his team at CSU, among many colleagues and programs, have been at the forefront of bringing research to fruition with biologic therapies. “We have built the largest orthopedic research center in a vet school anywhere in the world,” says McIlwraith, “And we’ve answered a lot of questions for horses, but there is still more questions to be answered.”
Perhaps one of the most exciting aspects of novel therapies are their place in not only the study of equine joint disease but also the translation to human medicine and back again. “We developed this vision with John and Leslie Malone for an institute for biologic translational therapies,” says McIlwraith. “John is interested in stem cells and asked to come see our data on them. We don’t often get an owner asking to see the data.” Drs. McIlwraith and Frisbie took John Malone through the data, and he was impressed, wanting to help facilitate a place where biologic therapies can continue to evolve, thrive and benefit both horses and people. Together with his wife, an avid equestrian, they made the largest donation ever to CSU to help create the Institute for Biologic Translational Therapies at CSU. “It’s very exciting,” says McIlwraith. “With horses, we have extra challenges when compared to humans because when the joint is worn out in humans you can get it replaced. We can’t do that with horses. We have to be treating them earlier and more effectively.”
In collaboration with MIT, Stanford, Pittsburgh and the University of Indiana, CSU has received funding from the National Institute of Health (NIH) because the horse has been recognized and accepted as an excellent model for humans. Due to their similar thickness of articular cartilage, equine joint research, particularly in biologic therapies, shows great promise in both species.
The Inspiration for Greatness
There’s no question that Wayne McIlwraith and Larry Bramlage have impacted the field of veterinary medicine in ways that will be felt for generations to come. They broke new ground, asked questions, found answers and did so while maintaining a deep loyalty to the horse. “I look back on my career and arthroscopy; I was involved in the developmental stages of the techniques,” says McIlwraith. “I wrote the first two editions of the book. But I’m still fascinated every time I go into a joint. I’ve probably done 15,000 horses and 25,000 joints, and I still think they’re really cool,” he says genuinely. “But really, I became a veterinarian because I wanted to treat animals and fix animals. That’s still what it’s all about.”
More than talent or a love of their profession, these two men have found the key to staying power. They remain interested, engaged, polished and at the top of their field with no plans to retire any time soon or ever. “One time a classmate of mine from school said, ‘how many ankle chips do you have to take out in your career?’ If that’s the way I looked at it, I’d be on the shelf already,” says Bramlage. “I’m stimulated by trying to understand the disease process, trying to intervene early and trying to make the joint come back to normal by what we do. If you don’t think deeper than just taking out an ankle chip for the surgery fee, you’re going to burn out in short order.” It’s an important insight into the constant interest, motivation and passion that drives men like this. “You have to be stimulated by the disease process,” Bramlage insists, “and wanting to unravel the disease process.” Like McIlwraith, he looks at his patients and feels invigorated and challenged. “The difference between success and failure, especially in the racehorse, is very small,” he says. “If that doesn’t challenge you to do this as perfectly as you can, knowing that having 95% of a racehorse is no better than none at all. That challenge has to make a difference to you.”
The future has been shaped by the two of them, their colleagues and the lasting impact they’ve made on new and exciting therapies for the equine joint. Ask McIlwraith, and he’ll tell you there’s no question that the future — the near future — holds incredible things. “I have a great research team here that we’ve built up from just one, me,” he says proudly. “They’re finding solutions, they’re smarter than me, they know more biology than me, and that’s equal fun for me.” With the research, the science, the accolades and the legacy, McIlwraith still looks back on his life’s work simply. “You see these horses perform, you have a happy horse, a happy owner and happy trainer, and it’s really good. That’s a pretty nice career.”
Veterinary medicine — whether you ask Larry Bramlage, Wayne McIlwraith or a veterinarian in their first year of practice — is a deep-seated passion. In the case of Bramlage and McIlwraith, they have dedicated much to the betterment of the equine joint. They brought about arthroscopy, as we know it, have helped bring biologic therapies mainstream and have laid the groundwork for future success. "To me, it's an avocation as well as a job," says Bramlage fondly. "Our pathways take different routes, partly by luck, partly by your own study and maybe a little bit by the hand of God or fate, whichever you believe in."

by Jessie Bengoa,
Platinum Performance®